What Is Vacuum Extraction?
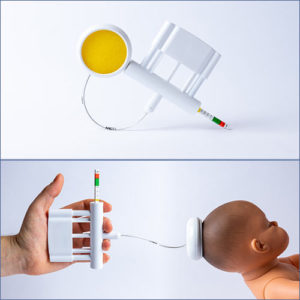
Vacuum extraction is a procedure used to assist a complicated or prolonged delivery. Obstetricians may choose to use vacuum extraction if they feel delivery complications could threaten the safety of the mother or baby.
The vacuum extraction device includes a soft cup that is firmly attached to the baby’s head and a vacuum pump to create suction.
Typically, the doctor will only gently pull while the mother pushes, so they work together with her contractions to help guide the baby through the birth canal.
Recent data shows that vacuum extraction was performed in 2.5% of U.S. births in 2021.
Vacuum extractions are only recommended during the second stage of labor when the cervix is fully dilated, and the baby has descended headfirst into the birth canal.
If doctors fail to safely perform a vacuum extraction delivery, babies can suffer from a wide range of health problems, including brain bleeds, cerebral palsy, and Erb’s palsy. Mothers can also be seriously injured.
You may qualify for financial assistance if you or your child experienced complications from a vacuum-assisted delivery. Get a free case review now for more details.
Reasons for Vacuum Delivery
When performed correctly, a vacuum extraction quickly removes the baby from the birth canal, reducing the risk of complications for the mother and their child.
- The baby’s heart rate is abnormal, indicating fetal distress.
- The mother has a health condition that prevents them from pushing for too long.
- The mother is pushing, but the baby is not descending.
- The mother is too tired to continue pushing.
In some cases, vacuum extraction eliminates the need for a cesarean section (C-section). However, a C-section is recommended if the doctor cannot safely deliver the baby with vacuum extraction.
What Causes Vacuum Extraction Complications?
An improperly performed assisted delivery is one of the top causes of vacuum extraction complications. The procedure should only be used if necessary since there is a higher risk to the baby and mother with a vacuum delivery than with natural birth.
Specifically, the mother is at risk of vacuum extraction complications like tailbone injury, tearing, and lacerations (cuts) in the vaginal area. This is because this type of delivery requires significant vaginal stretching for the baby to exit the birth canal.
The baby can suffer stretching or tearing of the nerves in their neck, putting them at risk of a spinal cord injury. Also, if too much suction is used during the vacuum extraction, it can injure the baby’s head and scalp.
Learn about the risks and complications of vacuum extraction during childbirth and what steps you can take if your baby was harmed. View Transcript.
Duration: 1 min 22 sec
Assistive devices like vacuum extractors can be necessary during a difficult delivery. However, even though most vacuum extractions are successful, this procedure can pose risks to both the mother and the child.
While vacuum extraction may be required in some vaginal deliveries, it should only be performed when there is a need to remove the baby from the birth canal quickly.
Serious complications can arise from vacuum deliveries, including brain damage, Erb’s palsy, skull fractures, and cephalohematomas. These complications can lead to developmental delays and permanent disability.
Sometimes, these complications are caused by doctors who misuse the vacuum device during delivery or fail to provide prompt and appropriate treatment after the procedure. These preventable medical mistakes are considered medical malpractice.
If your child suffered vacuum delivery complications due to medical negligence, you may be entitled to financial compensation. It’s important to explore your options and seek justice for any harm caused.
The Birth Injury Justice Center can help you connect with experienced birth injury lawyers and pursue financial assistance for medical negligence. Take action right now and protect your rights and your child’s future.
Some vacuum extraction complications cannot be avoided. However, they are often the result of improper use of the delivery tool, which can mean medical negligence occurred.
If you think your baby’s vacuum-assisted delivery complications could have been prevented, you probably have questions. One of our registered nurses can help. Connect with a labor and delivery nurse now in confidence.
Risk Factors for Vacuum Delivery Complications
There are specific risk factors that can lead to vacuum extraction injuries. Doctors and other medical providers must consider these risks when determining whether a vacuum delivery is appropriate.
- The baby has a bone or bleeding disorder.
- The baby’s head has not moved past the middle of the birth canal.
- The baby is too large to fit through the mother’s pelvis.
- The doctor cannot determine the position of the baby’s head.
- The mother is less than 34 weeks pregnant.
If any of these risk factors apply, a vacuum extractor should not be used to assist a vaginal birth.
Effects of Vacuum Extraction Complications
Vacuum extraction injuries that aren’t treated promptly can lead to various medical issues. Some vacuum extraction complications are minor and resolve immediately, but others may be more severe and last longer.
Short-Term Effects of Vacuum Delivery Complications
According to Cleveland Clinic, most vacuum extraction complications appear in the first 10 hours after birth.
Here are some of the short-term effects of vacuum delivery complications.
- Bleeding under the scalp (cephalohematoma)
- Bruising
- Newborn jaundice
- Swelling of the scalp (caput succedaneum)
- Difficulty urinating or incontinence (lack of control with urinating)
- Tailbone injury and pelvic pain
- Postpartum bleeding
- Vaginal tears
Most of these short-term vacuum delivery complications go away in a few days.
Long-Term Effects of Vacuum Delivery Complications
Long-term effects caused by vacuum extraction complications can be more severe and require ongoing medical treatment.
One of the most dangerous complications to the baby is bleeding in the brain, also known as an intraventricular hematoma.
This can happen when the vacuum cup pulls at the tissues of the baby’s head and ruptures fragile blood vessels, causing blood to pool under the scalp. This can add pressure to certain spaces of the brain, causing increased pressure on the brain’s nerves.
Newborn hematomas occur in about 10% of assisted deliveries.
The bleeding from a hematoma can also put pressure on the brain and its nerves, which can result in brain damage.
The brain and its nerves are the command center for the body, so pressure and damage to these areas can cause speech and developmental delays depending on what part of the brain is affected and the extent of the injury.
Other long-term effects for the baby may include:
- Cerebral palsy from brain damage
- Erb’s palsy or brachial plexus palsy
- Hearing loss
- Kernicterus
- Shoulder dystocia
- Skull fractures
It can be months or even years before the effects of vacuum delivery complications become noticeable. In particular, developmental delays may take longer to detect since the brain does not fully develop until the mid-to-late 20s.
Because of this, it’s important to monitor your child for symptoms of common birth injuries and ensure they’re hitting appropriate developmental goals.
Take our free milestones quiz now to see if your child is on track.
IS YOUR CHILD MISSING DEVELOPMENTAL MILESTONES?
Take Our Milestones Quiz
Taking note of your child’s physical, social, and emotional skills can help you determine if they potentially suffered from an injury at birth. An early diagnosis can help your child get the treatment they need as soon as possible.
Q1: How old is your child?
0-2 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child hold their head steadily on their own?
- Q3: Can your child push themselves up when they are lying on their stomach?
- Q4: Has your child started to make smoother movements with their arms and legs?
- Q5: Does your child smile at other people?
- Q6: Can your child bring their hands to their mouth?
- Q7: Does your child turn their head when they hear a noise?
- Q8: Does your child coo or make gurgling noises?
- Q9: Does your child follow things with their eyes?
- Q10: Does your child try to look at their parents or caregivers?
- Q11: Does your child show boredom, cry, or fuss when engaged in an activity that hasn’t changed in a while?


3-4 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child hold their head steadily on their own?
- Q3: Does your child push down on their legs when their feet are on a flat surface?
- Q4: Has your child started to roll over from their stomach to their back?
- Q5: Can your child hold and shake a toy such as a rattle?
- Q6: Does your child bring their hands to their mouth?
- Q7: Does your child play with people and start to cry when the playing stops?
- Q8: Does your child smile spontaneously, especially at people?
- Q9: Does your child copy some movements and facial expressions of other people?
- Q10: Does your child babble with expressions and copy sounds they hear?
- Q11: Does your child cry in different ways to show hunger, pain, or tiredness?
- Q12: Does your child respond to affection like hugging or kissing?
- Q13: Does your child follow moving things with their eyes from side to side?
- Q14: Does your child recognize familiar people at a distance?


5-6 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child roll over on both sides (front to back/back to front)?
- Q3: Has your child begun to sit without support?
- Q4: Does your child rock back and forth?
- Q5: Can your child support their weight on their legs (and perhaps bounce) when standing?
- Q6: Has your child begun to pass things from one hand to the other?
- Q7: Does your child bring objects such as toys to their mouth?
- Q8: Does your child know if someone is not familiar to them and is a stranger?
- Q9: Does your child respond to other people’s emotions, such as a smile or a frown?
- Q10: Does your child enjoy looking at themselves in the mirror?
- Q11: Does your child look at things around them?
- Q12: Does your child respond to sounds they hear by making sounds themselves?
- Q13: Does your child make sounds to show joy or displeasure?
- Q14: Does your child respond to their own name?
- Q15: Has your child started to string vowels together, such as "ah," "eh," or "oh," or started to say consonant sounds such as "m" or "b"?
- Q16: Has your child begun to laugh?


7-9 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child crawl?
- Q3: Can your child stand while holding on to something to support them?
- Q4: Can your child sit without support?
- Q5: Can your child pull themselves up to stand?
- Q6: Does your child play peekaboo?
- Q7: Can your child move things from one hand to the other?
- Q8: Can your child pick small things up, such as a piece of cereal, with their thumb and index finger?
- Q9: Does your child look for things that they see you hide?
- Q10: Does your child watch the path of something as it falls?
- Q11: Does your child show fear when around strangers?
- Q12: Does your child become clingy with adults who are familiar to them?
- Q13: Does your child have favorite toys?
- Q14: Does your child use their fingers to point?
- Q15: Does your child understand “no”?
- Q16: Does your child make a lot of repetitive sounds, such as “mamama” or “bababa”?
- Q17: Does your child copy the sounds and gestures of other people?


10-12 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child stand alone with no support?
- Q3: Does your child walk while holding on to furniture?
- Q4: Can your child take a few steps without holding on to anything?
- Q5: Can your child get into a sitting position without any help?
- Q6: Does your child bang two things together when playing?
- Q7: Does your child poke with their index finger?
- Q8: Has your child started to use things like hairbrushes or drinking cups correctly?
- Q9: Does your child find hidden objects easily?
- Q10: Does your child play peekaboo or pat-a-cake?
- Q11: Does your child become shy or nervous around strangers?
- Q12: Does your child repeat actions or sounds to get attention?
- Q13: Does your child put out an arm or leg to help when getting dressed?
- Q14: Does your child cry when a parent leaves the room?
- Q15: Does your child show that they have favorite things or people?
- Q16: Does your child show fear?
- Q17: Does your child say things such as “mama,” “dada,” or “uh-oh”?
- Q18: Does your child try to say the words you say?
- Q19: Has your child started to use gestures like waving or shaking their head “no”?


13-18 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child walk by themselves?
- Q3: Does your child walk up stairs and run?
- Q4: Does your child pull toys while walking?
- Q5: Can your child drink from a cup on their own?
- Q6: Can your child eat with a spoon on their own?
- Q7: Can your child help undress themselves?
- Q8: Does your child have occasional temper tantrums?
- Q9: Does your child show affection to familiar people?
- Q10: Does your child become clingy in new situations?
- Q11: Does your child explore their environment alone with parents close by?
- Q12: Can your child say several single words?
- Q13: Can your child say and shake their head “no”?
- Q14: Does your child point to show things to other people?
- Q15: Does your child scribble?
- Q16: Does your child know what ordinary products such as phones, spoons, and brushes are used for?
- Q17: Can your child follow one-step commands such as “sit down” or “stand up”?
- Q18: Does your child play with a doll or stuffed animal by pretending to feed it?


19-23 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Has your child begun to run?
- Q3: Has your child kicked a ball?
- Q4: Can your child climb down and onto furniture on their own?
- Q5: Can your child walk up and down stairs while holding on?
- Q6: Can your child stand on their tiptoes?
- Q7: Has your child thrown a ball overhand?
- Q8: Does your child copy others, especially people older than them?
- Q9: Does your child get excited around other children?
- Q10: Has your child shown more independence as they've aged?
- Q11: Does your child do what they were told not to do and become defiant?
- Q12: Does your child point to things when they are named?
- Q13: Does your child know names of familiar people or body parts?
- Q14: Does your child say 2 to 4-word sentences?
- Q15: Does your child repeat words they hear?
- Q16: Does your child complete sentences and rhymes in familiar books?
- Q17: Does your child name items in books, such as dogs, cats, and birds?
- Q18: Does your child play simple pretend games?
- Q19: Has your child started to use one hand more than the other?
- Q20: Has your child begun to sort shapes and colors?
- Q21: Does your child follow 2-step instructions, such as “pick up your hat and put it on your head?”


24+ MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child run easily?
- Q3: Can your child climb?
- Q4: Can your child walk up and down stairs with one foot on each step?
- Q5: Can your child dress and undress themselves?
- Q6: Does your child show affection for friends without being told?
- Q7: Does your child take turns when playing games?
- Q8: Does your child show concern when others are crying?
- Q9: Does your child understand the idea of “mine" and "theirs"?
- Q10: Does your child show many different emotions?
- Q11: Does your child copy adults and friends?
- Q12: Does your child separate easily from their parents?
- Q13: Does your child get upset when there is a major change in their routine?
- Q14: Does your child say words such as “I,” “me,” “we,” “you,” and some plural nouns?
- Q15: Can your child say their first name, age, and gender?
- Q16: Can your child carry on a conversation with 2 to 3 sentences?
- Q17: Can your child work toys with buttons and other moving parts?
- Q18: Does your child play pretend with dolls, animals, or people?
- Q19: Can your child finish 3 or 4 piece puzzles?
- Q20: Can your child copy a circle when drawing?
- Q21: Can your child turn pages of a book one page at a time?
- Q22: Can your child turn door handles?


Treatment for Vacuum Extraction Complications
Doctors should immediately examine mothers and their babies for any vacuum extraction complications. Many vacuum extraction injuries can be treated if addressed soon after delivery.

Mothers who experience severe vaginal tears or undergo an episiotomy (surgical incision in the perineum to enlarge the vagina) will require stitching. These stitches will dissolve on their own and do not need to be removed.
Mothers who experience incontinence may require a catheter to drain their bladder for up to 24 hours. After the catheter is removed, they will be instructed to drink lots of water to stay hydrated and prevent urination problems.
After a difficult birth, some mothers may need a short-term catheter if they can’t urinate due to swelling. If urination isn’t possible within 6 hours of removing the catheter, it may be reinserted. Frequent catheter use raises infection risk.
Vacuum Delivery Complications and Medical Malpractice
Because of their professional experience and training, doctors are responsible for determining the best way to assist with a vaginal delivery. For this reason, the improper use of vacuum extractors may be considered medical malpractice.
Medical malpractice resulting in vacuum delivery complications can be caused by misusing the vacuum device during delivery or failing to provide prompt and appropriate treatment after the procedure.
Doctors should monitor the mother and newborn for any signs of vacuum extraction complications. Prompt treatment of jaundice, skull fractures, hematomas, and nerve damage can prevent a baby from developing serious health conditions.
When a baby suffers long-term complications from vacuum delivery, many families choose to pursue justice against negligent medical staff with the help of an experienced birth injury lawyer.
We’ve partnered with experienced birth injury lawyers who have helped families recover $862 million for preventable birth injuries — and they’re ready to help yours too.
Find Out If You’re Eligible for Financial Compensation
Vacuum extraction complications are preventable when medical professionals follow care guidelines correctly and provide prompt treatment to mothers and their babies. You may have a case for medical negligence if your doctor did not take the proper precautions during your vacuum extraction.
If your child suffered complications from a vacuum extraction, you may be able to receive compensation through a birth injury lawsuit.
Get a free case review today to learn how an experienced birth injury attorney may be able to help you and your family.
Vacuum Extraction Complications FAQs
What is vacuum extraction?
Vacuum extraction (also called a ventouse) is an assistive delivery method used during childbirth to guide a baby through the birth canal. It is performed during the second stage of labor, when the mother is pushing the baby out.
This method works in tandem with the mother’s pushing efforts rather than pulling the baby out directly.
What are the potential complications of vacuum extraction?
Examples of vacuum-assisted delivery complications include scalp injuries such as bruising or swelling, as well as skull fractures.
In some cases, a condition called intracranial hemorrhage, which is bleeding inside the skull, can occur. This condition is considered severe. Any time a baby’s brain is harmed, there is a risk for brain damage.
What is the most serious complication of vacuum extraction?
According to Cleveland Clinic, the most serious vacuum extraction complications include skull fractures and intracranial hemorrhage, which can lead to brain damage. Additionally, subgaleal hemorrhage (bleeding between the scalp and skull) can lead to death if left untreated.
Can vacuum delivery cause brain damage?
Yes, vacuum extraction complications can cause brain damage. If the vacuum suction device isn’t placed on the baby’s head correctly or too much pressure is applied, it can seriously damage a newborn baby’s brain.
Brain damage can also occur from lack of oxygen due to a vacuum-related injury like shoulder dystocia (when the baby’s shoulder gets lodged behind the mother’s pubic bone). In these situations, the head is delivered, but the shoulders are stuck, creating pressure on the baby and a lack of oxygen to the brain.
Some vacuum extraction can cause brain bleeds, which can put pressure on the brain and damage it.
How long does it take to heal from a vacuum delivery?
Most women recover from a vacuum delivery within 6 weeks if there are no complications.
Babies with bruises or swelling from vacuum extraction usually take a few weeks to heal. In the meantime, monitoring the baby’s head while it heals and attending regular follow-up appointments is important.
How long does it take for a baby's head to round after vacuum extraction?
The suction cup used in vacuum extraction can cause a baby’s head to swell into a cone shape. However, the baby’s head should start to round (return to its normal shape) 2-3 days after birth.
Which is better: vacuum or forceps?
Both vacuum extraction and forceps delivery have advantages and disadvantages. Some studies have shown that rates of shoulder dystocia and newborn cephalohematoma are lower in babies delivered by vacuum extraction versus forceps.
On the other hand, these studies also found that the risk of maternal complications — especially vaginal tears — is higher with the use of forceps.
Doctors are responsible for choosing the assistive device that is best for the mother and baby.