Common Erb’s Palsy Treatment Options
Erb’s palsy occurs when the brachial plexus network of nerves is injured during childbirth. This can happen when a doctor or nurse uses excessive force on the arm, shoulder, or neck when pulling a baby out of the birth canal during a difficult delivery.

Treatments for brachial plexus injuries can vary depending on the severity of nerve damage. Neuropraxias, the mildest type of traumatic nerve damage injury, clears up on its own at three months of age. More severe injuries, such as avulsions (where the nerve is torn apart from the spinal cord), may require intensive treatment.
Erb’s palsy treatment options generally include physical therapy and occupational therapy for mild cases and more intensive surgery for more severe cases.
Your doctor will recommend a treatment plan that is best for your child’s particular case of Erb’s palsy to give them the best chance of recovery. The treatments used will depend on your child’s condition and symptoms.
It is important to seek Erb’s palsy treatments as soon as your child is diagnosed to reduce the chance of long-term or permanent disability.
Physical Therapy for Erb’s Palsy
Physical therapy is the primary treatment method for Erb’s palsy. Physical therapy helps children regain strength and control in their affected arm, allowing many patients to heal without other treatment methods.
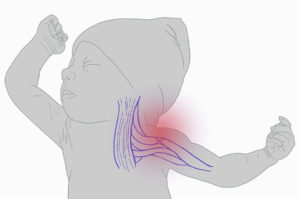 Erb’s palsy physical therapy can start as early as two weeks after the child is born. However, if your child is diagnosed at birth, your medical provider will likely provide you with a list of guidelines for handling your child so that you do not harm their affected arm before they start therapy.
Erb’s palsy physical therapy can start as early as two weeks after the child is born. However, if your child is diagnosed at birth, your medical provider will likely provide you with a list of guidelines for handling your child so that you do not harm their affected arm before they start therapy.
These guidelines include the following:
- Do not lift the child under their arms.
- Protect their affected arm by carefully handling the baby.
- When dressing the child, place their affected arm into the sleeve first, followed by their head and unaffected arm.
Due to inflammation in the affected area, it is essential to follow these guidelines in the days following the injury until physical therapy can commence. Many children with Erb’s palsy can partially or fully recover with physical therapy.
Erb’s Palsy Physical Therapy After Two Weeks of Age
Once a child with Erb’s palsy is two weeks old, they can begin intensive physical therapy for their affected arm or shoulder.
In these cases, the treatment is typically conducted with a licensed physical therapist on a weekly or biweekly basis.
Physical therapy for Erb’s palsy can help relieve stiffness and restore the range of motion in the child’s affected arm. Physical therapists will use several different range-of-motion exercises, equipment, and massage therapy techniques to help babies regain strength.
Physical therapy treatment techniques can vary depending on the child’s specific needs and the severity of the injury. The physical therapist may also provide parents with additional physical therapy instruction to complete at home.
The treatment usually involves the following:
- Adaptive equipment, like splints to prevent contractures (stiffening of the joint or muscles)
- Daily home-based stretching and exercise
- Gentle passive motion of joints
- Monthly follow-up at a clinic
- Weekly or biweekly formal physical therapy
If you believe a preventable birth injury caused your child’s Erb’s palsy, talk to one of our caring registered nurses to learn more about your next steps.

“We have attorneys across the country who can help your family seek justice and compensation to cover lifelong treatment costs.”
— Kristin Proctor, RNC-OB, On-Staff Registered Nurse
Occupational Therapy for Erb’s Palsy
Most newborns with brachial plexus birth palsy are likely to recover naturally, but recovery is slow, often taking up to two years. During this time, a child’s doctor will regularly monitor the progress of nerve recovery and may recommend occupational therapy.
Occupational therapy is a key treatment to improve fine motor skills in the affected arm. Erb’s palsy can significantly impair a child’s use of their arm, wrist, hand, and/or shoulder, hindering their ability to perform everyday tasks.
In occupational therapy, therapists use various techniques to lessen muscle weakness and enhance motor skills.
Occupational therapy can help children complete daily activities such as:
- Bathing
- Brushing teeth/hair
- Drawing
- Drinking from a cup
- Eating with utensils
- Getting dressed
- Writing
The overall goal of Erb’s palsy occupational therapy is to help children become as independent as possible. Starting occupational therapy early may improve the quality of life for children with Erb’s palsy.
IS YOUR CHILD MISSING DEVELOPMENTAL MILESTONES?
Take Our Milestones Quiz
Taking note of your child’s physical, social, and emotional skills can help you determine if they potentially suffered from an injury at birth. An early diagnosis can help your child get the treatment they need as soon as possible.
Q1: How old is your child?
0-2 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child hold their head steadily on their own?
- Q3: Can your child push themselves up when they are lying on their stomach?
- Q4: Has your child started to make smoother movements with their arms and legs?
- Q5: Does your child smile at other people?
- Q6: Can your child bring their hands to their mouth?
- Q7: Does your child turn their head when they hear a noise?
- Q8: Does your child coo or make gurgling noises?
- Q9: Does your child follow things with their eyes?
- Q10: Does your child try to look at their parents or caregivers?
- Q11: Does your child show boredom, cry, or fuss when engaged in an activity that hasn’t changed in a while?


3-4 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child hold their head steadily on their own?
- Q3: Does your child push down on their legs when their feet are on a flat surface?
- Q4: Has your child started to roll over from their stomach to their back?
- Q5: Can your child hold and shake a toy such as a rattle?
- Q6: Does your child bring their hands to their mouth?
- Q7: Does your child play with people and start to cry when the playing stops?
- Q8: Does your child smile spontaneously, especially at people?
- Q9: Does your child copy some movements and facial expressions of other people?
- Q10: Does your child babble with expressions and copy sounds they hear?
- Q11: Does your child cry in different ways to show hunger, pain, or tiredness?
- Q12: Does your child respond to affection like hugging or kissing?
- Q13: Does your child follow moving things with their eyes from side to side?
- Q14: Does your child recognize familiar people at a distance?


5-6 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child roll over on both sides (front to back/back to front)?
- Q3: Has your child begun to sit without support?
- Q4: Does your child rock back and forth?
- Q5: Can your child support their weight on their legs (and perhaps bounce) when standing?
- Q6: Has your child begun to pass things from one hand to the other?
- Q7: Does your child bring objects such as toys to their mouth?
- Q8: Does your child know if someone is not familiar to them and is a stranger?
- Q9: Does your child respond to other people’s emotions, such as a smile or a frown?
- Q10: Does your child enjoy looking at themselves in the mirror?
- Q11: Does your child look at things around them?
- Q12: Does your child respond to sounds they hear by making sounds themselves?
- Q13: Does your child make sounds to show joy or displeasure?
- Q14: Does your child respond to their own name?
- Q15: Has your child started to string vowels together, such as "ah," "eh," or "oh," or started to say consonant sounds such as "m" or "b"?
- Q16: Has your child begun to laugh?


7-9 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child crawl?
- Q3: Can your child stand while holding on to something to support them?
- Q4: Can your child sit without support?
- Q5: Can your child pull themselves up to stand?
- Q6: Does your child play peekaboo?
- Q7: Can your child move things from one hand to the other?
- Q8: Can your child pick small things up, such as a piece of cereal, with their thumb and index finger?
- Q9: Does your child look for things that they see you hide?
- Q10: Does your child watch the path of something as it falls?
- Q11: Does your child show fear when around strangers?
- Q12: Does your child become clingy with adults who are familiar to them?
- Q13: Does your child have favorite toys?
- Q14: Does your child use their fingers to point?
- Q15: Does your child understand “no”?
- Q16: Does your child make a lot of repetitive sounds, such as “mamama” or “bababa”?
- Q17: Does your child copy the sounds and gestures of other people?


10-12 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child stand alone with no support?
- Q3: Does your child walk while holding on to furniture?
- Q4: Can your child take a few steps without holding on to anything?
- Q5: Can your child get into a sitting position without any help?
- Q6: Does your child bang two things together when playing?
- Q7: Does your child poke with their index finger?
- Q8: Has your child started to use things like hairbrushes or drinking cups correctly?
- Q9: Does your child find hidden objects easily?
- Q10: Does your child play peekaboo or pat-a-cake?
- Q11: Does your child become shy or nervous around strangers?
- Q12: Does your child repeat actions or sounds to get attention?
- Q13: Does your child put out an arm or leg to help when getting dressed?
- Q14: Does your child cry when a parent leaves the room?
- Q15: Does your child show that they have favorite things or people?
- Q16: Does your child show fear?
- Q17: Does your child say things such as “mama,” “dada,” or “uh-oh”?
- Q18: Does your child try to say the words you say?
- Q19: Has your child started to use gestures like waving or shaking their head “no”?


13-18 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child walk by themselves?
- Q3: Does your child walk up stairs and run?
- Q4: Does your child pull toys while walking?
- Q5: Can your child drink from a cup on their own?
- Q6: Can your child eat with a spoon on their own?
- Q7: Can your child help undress themselves?
- Q8: Does your child have occasional temper tantrums?
- Q9: Does your child show affection to familiar people?
- Q10: Does your child become clingy in new situations?
- Q11: Does your child explore their environment alone with parents close by?
- Q12: Can your child say several single words?
- Q13: Can your child say and shake their head “no”?
- Q14: Does your child point to show things to other people?
- Q15: Does your child scribble?
- Q16: Does your child know what ordinary products such as phones, spoons, and brushes are used for?
- Q17: Can your child follow one-step commands such as “sit down” or “stand up”?
- Q18: Does your child play with a doll or stuffed animal by pretending to feed it?


19-23 MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Has your child begun to run?
- Q3: Has your child kicked a ball?
- Q4: Can your child climb down and onto furniture on their own?
- Q5: Can your child walk up and down stairs while holding on?
- Q6: Can your child stand on their tiptoes?
- Q7: Has your child thrown a ball overhand?
- Q8: Does your child copy others, especially people older than them?
- Q9: Does your child get excited around other children?
- Q10: Has your child shown more independence as they've aged?
- Q11: Does your child do what they were told not to do and become defiant?
- Q12: Does your child point to things when they are named?
- Q13: Does your child know names of familiar people or body parts?
- Q14: Does your child say 2 to 4-word sentences?
- Q15: Does your child repeat words they hear?
- Q16: Does your child complete sentences and rhymes in familiar books?
- Q17: Does your child name items in books, such as dogs, cats, and birds?
- Q18: Does your child play simple pretend games?
- Q19: Has your child started to use one hand more than the other?
- Q20: Has your child begun to sort shapes and colors?
- Q21: Does your child follow 2-step instructions, such as “pick up your hat and put it on your head?”


24+ MONTHS DEVELOPMENTAL MILESTONES QUIZ
- Q2: Can your child run easily?
- Q3: Can your child climb?
- Q4: Can your child walk up and down stairs with one foot on each step?
- Q5: Can your child dress and undress themselves?
- Q6: Does your child show affection for friends without being told?
- Q7: Does your child take turns when playing games?
- Q8: Does your child show concern when others are crying?
- Q9: Does your child understand the idea of “mine" and "theirs"?
- Q10: Does your child show many different emotions?
- Q11: Does your child copy adults and friends?
- Q12: Does your child separate easily from their parents?
- Q13: Does your child get upset when there is a major change in their routine?
- Q14: Does your child say words such as “I,” “me,” “we,” “you,” and some plural nouns?
- Q15: Can your child say their first name, age, and gender?
- Q16: Can your child carry on a conversation with 2 to 3 sentences?
- Q17: Can your child work toys with buttons and other moving parts?
- Q18: Does your child play pretend with dolls, animals, or people?
- Q19: Can your child finish 3 or 4 piece puzzles?
- Q20: Can your child copy a circle when drawing?
- Q21: Can your child turn pages of a book one page at a time?
- Q22: Can your child turn door handles?


Surgery for Erb’s Palsy
Some children with more severe cases of Erb’s palsy may require surgery alongside physical and occupational therapy to repair damaged nerves.
The goal of brachial plexus birth palsy surgery is to regain range of motion and control of the affected shoulder, upper arm, wrist, and/or hand. There are several surgical options available, depending on the child’s needs.

In very severe cases of Erb’s palsy affecting the hand, some doctors may recommend microsurgical neurolysis, or nerve surgery. However, this procedure is considered controversial and may not help a patient recover hand function.
Although surgery is successful for most patients with severe cases of Erb’s palsy, it can take several months for a child to regain full control of the muscles in their arm and lower hand.
During this time, doctors will recommend that the child continue physical therapy and medical evaluation.
Prognosis After Erb’s Palsy Treatment
Treatment for an Erb’s palsy nerve injury varies based on the severity of the condition. Fortunately, children diagnosed with Erb’s palsy have a great chance of complete recovery.
The majority of children with Erb’s palsy will regain full control of their arm through physical therapy. Only a small percentage of children will require surgery, and an even smaller percentage will have lifelong symptoms.
The American Academy of Orthopedic Surgeons (AAOS) recommends frequent medical checkups for a baby with Erb’s palsy to determine if the nerves are healing. It may take up to two years for symptoms to lessen.
After Erb’s palsy has been diagnosed, it is key to start treatment as quickly as possible to increase your child’s chances of a full recovery.
Get Help Paying For Erb’s Palsy Treatment Today
Health care professionals have a duty to safely deliver babies, even during emergency birthing situations. However, Erb’s palsy is often caused by preventable injuries during childbirth.
Many children with Erb’s palsy can make a full recovery with prompt treatment. If your child’s condition was caused by medical negligence, you should not have to pay for their treatment.
Your family may be eligible for financial compensation if your child’s injury was preventable. This compensation can help cover your child’s medical costs and Erb’s palsy treatment.
To learn more about taking legal action, call us at (800) 914-1562 or get a free case review.
Erb’s Palsy Treatment FAQs
Erb’s palsy (also called Erb-Duchenne palsy) is caused by using excessive force while pulling or twisting on the child’s arm, shoulder, or neck when exiting the birth canal.
There are several risk factors that can lead to Erb’s palsy, such as the fetus being in a breech position (legs first), shoulder dystocia (one or both shoulders stuck in the birth canal), and more.
Many children are able to make a partial or full recovery from Erb’s palsy with prompt treatment.
According to the AAOS, about 80% of children with Erb’s palsy make a full recovery with treatment.
Most cases of Erb’s palsy are treated with physical therapy that focuses on regaining muscle control and strength.
More severe cases of Erb’s palsy may be treated with a combination of physical therapy and surgery.
Nerve damage and Erb’s palsy symptoms could worsen if the condition is left untreated. This may result in permanent brachial plexus damage, which can greatly affect the child’s motor skills and quality of life.
It is critical to seek Erb’s palsy treatment as soon as your child is diagnosed with the condition to give them the best chance at fully recovering.






