What Is a Newborn Cephalohematoma?
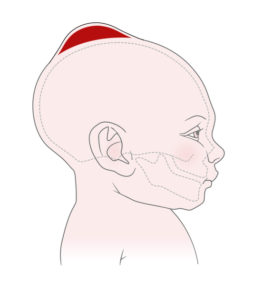 A newborn cephalohematoma is a buildup of ruptured blood vessels (hemorrhage) in the periosteum (the tissue that covers the skull).
A newborn cephalohematoma is a buildup of ruptured blood vessels (hemorrhage) in the periosteum (the tissue that covers the skull).
In a hematoma, blood pools outside the blood vessels and is visible on the baby’s scalp.
The pooled blood puts pressure on brain tissue, which may lead to fatal complications or lifelong disability if not immediately diagnosed and treated.
According to experts at the University at Buffalo and Thomas Jefferson University Hospital, infant hematomas occur in 0.4% to 2.5% of all live births.
This type of birth injury is fairly common and many cases will heal on their own. In rare cases, however, severe infant hematomas can lead to complications or death without proper treatment.
If your child suffered from newborn cephalohematoma, reach out to one of our experienced registered nurses to get help today. You may be entitled to seek newborn cephalohematoma compensation.
Cephalohematoma vs. Caput Succedaneum
While both cause swelling on a newborn’s head, cephalohematoma and caput succedaneum are different. A newborn cephalohematoma involves ruptured blood vessels under the scalp, and caput succedaneum is classified as swelling of the scalp itself.
Caput succedaneum usually results from pressure placed on the scalp during a head-first delivery. It is more common in long or difficult deliveries and/or when vacuum extraction is needed.
Unlike a newborn cephalohematoma, which can take months to go away, the swelling from caput succedaneum usually requires no treatment and disappears within three days.
Types of Newborn Cephalohematomas
Medical professionals categorize newborn cephalohematomas based on when symptoms begin to appear.
The two categories of infant hematoma include:
- Acute infant hematoma: Symptoms will appear immediately or within hours of delivery.
- Chronic infant hematoma: Symptoms may not appear until days or weeks after birth.
If acute infant hematoma is not treated properly, it can lead to chronic infant hematoma.
Diagnosing the condition early on may improve the outcome. Without proper diagnosis and treatment, both types of newborn cephalohematoma can cause complications that lead to brain damage or even death.
What Are the Most Common Newborn Cephalohematoma Causes?
Head injuries that take place during childbirth cause newborn hematomas. These injuries may occur because the baby’s head was pushed against their mother’s pelvis.
Other times, newborn hematomas happen due to complications from the use of forceps or vacuum extractors.
Learn about newborn cephalohematoma, the buildup of ruptured blood vessels on the scalp, and what to do if your baby was harmed during childbirth. View Transcript.
Duration: 1 min 06 sec
A newborn cephalohematoma is a birth injury caused by trauma to an infant’s head during childbirth.
Also known as an infant hematoma or newborn hematoma, it results from trauma to the baby’s head during delivery.
While many cases of infant cephalohematoma get better on their own, some babies require medical attention.
In certain situations, doctors may need to perform surgery to address skull deformities or other potential complications.
If you believe your baby’s birth injury was caused by medical malpractice, it’s essential to take action.
You have the right to seek justice and compensation for your child’s pain and suffering. Get a free consultation today to determine if medical malpractice played a role in your child’s birth injury.
The experienced birth injury attorneys in our network can review your case and guide you through the legal process.
Your child’s well-being is our priority. Let the Birth Injury Justice Center help you fight for their rights
Overall, a newborn cephalohematoma birth injury is often a sign of difficult labor. The longer it takes to deliver a baby, the longer the baby’s head may be compressed by the birth canal, increasing the risk of a newborn hematoma.
Infant hematomas may also occur due to the infant’s size and position or an act of medical negligence. Get a free case review today if you believe your child’s birth injury was caused by medical malpractice.
Assisted-Delivery Devices
Doctors sometimes decide to use devices such as forceps or a vacuum to aid in deliveries that are longer or more difficult than usual.
These delivery tools grip the baby’s head and allow doctors to move the infant through the birth canal.
However, because of the pressure they place on the baby’s head, assistive devices can end up rupturing the fragile blood vessels beneath the scalp and causing a cephalohematoma.
Infant Size
A newborn cephalohematoma is more likely to occur in larger infants, particularly males. Babies who weigh more than 8 pounds, 13 ounces may have trouble moving through the birth canal and take longer to be delivered.
The stress caused by the compression on a larger baby’s head in the birth canal puts them at greater risk for a cephalohematoma.
On the other hand, average-sized fetuses can also experience increased compression if the mother has a smaller-than-normal pelvis.
Medical Negligence
Doctors are trained to detect and reduce the risks of newborn cephalohematoma. If a risk is identified, your doctor should take actions to decrease the chances of a potential injury and monitor your baby for a hematoma after delivery.
If the doctor does not follow protocol and your child does not receive prompt medical intervention, it may be considered medical negligence. Misusing assistive tools during delivery or failing to address fetal distress quickly can qualify as negligence or malpractice.
In cases of medical malpractice, compensation may be available to you and your family.
Newborn Cephalohematoma Risk Factors
The most commonly reported risk factor for an infant hematoma is using vacuum extractors or forceps during childbirth.
Other newborn cephalohematoma risk factors include:
- Breech (feet-first) or posterior (face-up) delivery
- Carrying multiple babies (twins, triplets, or more)
- Difficult or prolonged labor
- Epidural pain relief during childbirth
- Mother’s inability to push the child through the birth canal
- Premature birth
Doctors and medical staff who fail to recognize potential risk factors for newborn cephalohematoma may be liable for any complications that occur as a result.
If your baby suffered a head injury during childbirth that you believe could have been prevented, contact us today to learn what you can do next.
Newborn Cephalohematoma Complications
Certain health complications may arise if your newborn develops a cephalohematoma. It is important to know the signs and symptoms of each, as some complications may cause your baby to suffer long-term consequences.
Anemia
The human body needs a healthy amount of red blood cells to carry oxygen to the organs and tissues. Anemia occurs when there is a shortage of these red blood cells.
Since a cephalohematoma causes blood to pool away from the baby’s circulatory system, it can lead to low red-blood-cell count. Larger cephalohematomas are more likely to cause anemia.
Your baby may be anemic if they have:
- An abnormally fast heartbeat
- Trouble breathing
- An unhealthy skin tone
Some anemic babies may need a blood transfusion to maintain healthy oxygen levels.
Calcified Cephalohematoma
If a newborn cephalohematoma does not go away after about a month, the hematoma may become calcified. Calcification is when bone deposits form and harden around the pool of blood.
Although uncommon, severe cases of cephalohematoma calcification can cause the child’s skull to become misshapen. Most babies will need corrective surgery to remove calcification.
Infection
One of the more dangerous complications of newborn cephalohematoma is the risk of neonatal infection.
Infection can begin in the pooled blood and lead to a serious systemic infection such as sepsis or meningitis.
These types of serious infections have a high death rate in infants, so prompt diagnosis is critical.
Jaundice
Jaundice is caused when there is an excess of bilirubin, which is an orange-yellow chemical waste created by recycled blood cells. Bilirubin is normally disposed of through the liver or excreted in feces or urine.
Babies with jaundice usually have yellowing of the skin and eyes.
Severe cases of untreated jaundice can cause kernicterus, a serious condition that can result in brain damage or death in some cases.
Skull Fractures
Skull fractures are a more common complication of newborn cephalohematoma.
Fortunately, skull fractures are usually not very serious and often heal without treatment.
Fractures occur in almost 25% of newborn cephalohematoma cases, according to the journal Academic Forensic Pathology.
Newborn Cephalohematoma Symptoms
Your child may develop signs and symptoms of an infant hematoma right after the injury occurred, or it may take days or weeks for symptoms to appear. The time between the injury and the appearance of symptoms is referred to as the lucid interval.
The most common symptom of a cephalohematoma is a soft bump or bulge on your baby’s head.
Other signs and symptoms of newborn cephalohematoma include:
- Feeding difficulties
- High-pitched crying
- Increased head circumference
- Pain in the skull area
- Seizures
- Swelling
- Tiredness
- Vomiting
It’s important to note that bruising and hematomas are commonly mistaken for one another. The collection of blood in a hematoma can create a dark spot on your baby’s skin, similar to a bruise.
While bruises typically show up a few hours after a child suffers a minor injury, cephalohematomas appear only after head trauma.
Compensation from a malpractice claim can help your family cover birth injury treatment costs.
Newborn Cephalohematoma Diagnosis
If your child is showing symptoms of newborn cephalohematoma, your doctor will monitor your child’s head size to see if it is expanding more quickly than it should.


Next, your doctor will likely order imaging scans. They will often choose to do a computed tomography (CT) scan. The doctor may also recommend an X-ray or magnetic resonance imaging (MRI).
These imaging tests will help the doctor pinpoint the source of the bleeding and the size of the hematoma.
Newborn Cephalohematoma Prognosis
If treated properly, babies diagnosed with newborn cephalohematoma will recover in a few months. Most cephalohematomas heal on their own without causing long-term physical or developmental challenges.
Usually, the middle of the hematoma will start to disappear first. The outer rim may harden due to calcium.
Many of the complications related to newborn cephalohematomas can be avoided or reduced if the injury is caught and treated early.
For this reason, if your doctor or nurse fails to address the signs of an infant hematoma quickly enough, it may be considered medical malpractice.
Newborn Cephalohematoma Treatment
If you suspect your child has a newborn hematoma, seek immediate medical attention. Your child may need surgery to drain blood, remove a large clot, or tie off a bleeding vein. In cases where surgery is not needed, treatment involves a lot of resting.
Treatments for possible complications caused by a hematoma include:
- Anemia: Blood transfusion, phototherapy, or antibiotics
- Calcification: Surgery
- Infection: Antibiotics
- Jaundice: Monitoring and light therapy
- Skull fracture: Careful monitoring to ensure it heals properly
With treatment, a hematoma does not generally cause major problems to most newborns. Speak with your doctor to learn their specific instructions for recovering from newborn cephalohematoma.
Get Help for Newborn Cephalohematoma Caused by Medical Negligence
If your child’s hematoma was caused by improper care during childbirth, you and your family may be entitled to financial compensation.
Although pursuing legal action will not undo the harm caused to your child, the compensation a newborn cephalohematoma lawyer may be able to secure for you can help cover your child’s ongoing treatment. It can also help hold the responsible parties accountable for their acts of medical negligence.
To connect with a law firm experienced in birth injury cases, contact the Birth Injury Justice Center today for a free case review.
Newborn Cephalohematoma FAQs
Is cephalohematoma normal in newborns?
Yes, cephalohematomas are fairly common in newborns (around 2.5% of babies delivered with a prolonged vaginal birth will get them). The lumps caused by cephalohematomas usually disappear on their own without needing treatment.
However, doctors should continue to monitor the hematoma after birth for any signs of calcification (hardened bone deposits). Severe calcification can cause permanent deformities in the baby’s skull.
How long does it take for a cephalohematoma to resolve in a newborn?
The bruising and blood buildup caused by a newborn cephalohematoma should go away without treatment in a couple of weeks or months, according to the Cleveland Clinic.
However, if a cephalohematoma does not heal within four weeks, it could begin to calcify. Often the middle of the hematoma will start to disappear first while the outer rim gets harder (from calcium).
Severe calcification may result in complications like permanent skull deformity that may require surgery to fix.
Will rubbing a hematoma on a baby's head help it to go away?
No, rubbing a newborn baby’s cephalohematoma won’t make it go away. The lump from a cephalohematoma usually heals on its own with no treatment needed.
It’s best to avoid rubbing or applying pressure on a hematoma so that the ruptured blood vessels can heal properly.
Can a cephalohematoma cause brain damage?
No, a cephalohematoma alone does not usually cause brain damage since the blood is pooled on top of the skull.
However, babies who are born with a cephalohematoma may be at risk for certain medical complications like jaundice, which can cause brain damage in severe cases that are left untreated.